Cystic fibrosis and the lungs - symptoms and treatment
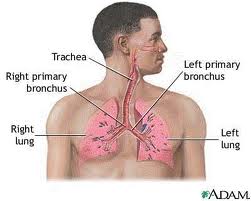
Cystic fibrosis is an inherited genetic disorder affecting mucus production and clearance, CYSTIC FIBROSIS alters the functioning of exocrine glands throughout the body and affects nearly all of the body’s systems. In the LUNGS, cystic fibrosis causes changes in the consistency and composition of the mucus the lungs secrete. The mucus accumulates along the inner walls of the bronchi, causing irritation and INFLAMMATION that eventually thickens the walls of the bronchi. The mucus becomes thick, creating obstructions in the bronchi that reduce air flow and eventually produce regions of ATELECTASIS (collapsed bronchial segments). The plugs of thickened mucus also attract BACTERIA, resulting in recurrent INFECTION that manifest as BRONCHITIS and PNEUMONIA.
Health experts estimate that about 3 percent of the population in the United States carries the recessive GENE MUTATION for cystic fibrosis. The disorder is 5 to 10 times more common among whites than among other racial populations. Even one generation ago, cystic fibrosis typically caused death by late ADOLESCENCE. Current treatment methods and early diagnosis has extended life expectancy into the 30s for most people who have cystic fibrosis, and many live longer. Cystic fibrosis nearly always affects the lungs and requires continuous therapy to maintain adequate BREATHING and oxygenation.
Symptoms of Cystic Fibrosis and Diagnostic Path
The symptoms of cystic fibrosis vary according to the body system first affected and usually appear in childhood. Chronic productive COUGH, recurrent bronchitis or pneumonia, and pronounced wheezing are among the indications of pulmonary involvement. The diagnostic path includes chest Xrays and pulmonary function tests, which demonstrate changes in lung structure and function characteristic of cystic fibrosis. Other diagnostic procedures look for nonpulmonary indications of cystic fibrosis such as sinus disease, pancreatic disease, decreased BONE DENSITY, and INFERTILITY. Family history of cystic fibrosis provides strong suspicion of the diagnosis. A positive sweat chloride test and GENETIC TESTING that identifies cystic fibrosis mutations. This provides conclusive diagnosis.
Cystic Fibrosis Treatment Options and Outlook
Treatment requires close coordination to target symptoms and disease developments across body systems. Pulmonary treatment aims to keep the airways as open as possible and to prevent infection, or treat infection early and aggressively. IMMUNIZATION to protect against CHILDHOOD DISEASES such as PERTUSSIS (whooping cough), CHICKENPOX, and MEASLES are crucial, as are annual INFLUENZA immunizations (flu shots) and pneumonia vaccination every five years at all ages. CHEST PERCUSSION AND POSTURAL DRAINAGE help clear the airways of mucus accumulations. Though coughing is a frustrating symptom, it is also an important function for removing mucus from the chest. Bronchodilators help improve functioning of the airways and removal of mucus from them.
Moderate to high doses of the NONSTEROIDAL ANTI-INFLAMMATORY DRUG (NSAID) ibuprofen (Advil or Motrin) taken regularly may slow bronchial inflammation and damage in many people, especially children. CORTICOSTEROID MEDICATIONS become necessary when ibuprofen can no longer control the inflammation or when inflammation becomes widespread in the lungs. ANTIBIOTIC MEDICATIONS become necessary to treat infections. People who have cystic fibrosis commonly acquire antibioticresistant bacteria, which may necessitate treatment with more powerful intravenous antibiotics. Inhaled antibiotic therapies are also becoming available for treatment as well as prophylaxis (prevention).
Cystic fibrosis has numerous nonpulmonary complications that also require close attention. Dysfunction of the PANCREAS results in malabsorption that may necessitate nutritional support. The nature and severity of symptoms vary widely among individuals. Cystic fibrosis is progressive, however, and these treatments are only supportive. When they fail, bilateral LUNG TRANSPLANTATION is the final, though high-risk, treatment option.
Cystic Fibrosis Risk Factors and Preventive Measures
The only risk factor for cystic fibrosis is the recessive gene mutation. Because this mutation is relatively prevalent in the American population, many people do not know they carry it until a child develops the disease. Genetic testing and GENETIC COUNSELING may be helpful for people who have family histories of cystic fibrosis.
See also ANTIBIOTIC PROPHYLAXIS; ANTIBIOTIC RESISTANCE; GENETIC DISORDERS; INHERITANCE PATTERNS; ORGAN TRANSPLANTATION.